Challenges in the Vascular Approach of Transfemoral Transcatheter Aortic Valve Implantation
In order to successfully perform transfemoral TAVI, the operators should not only have appropriate knowledge on the devices they use and good training in femoral 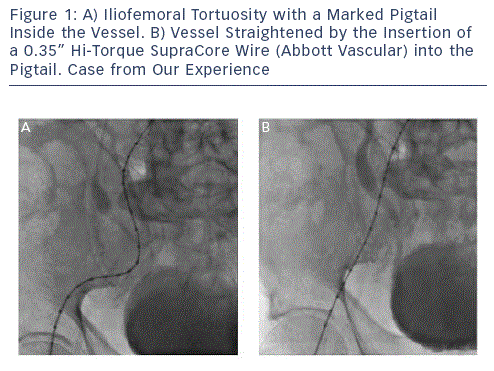 access and management of its specic complications, but they should also perform comprehensive screening of patients and careful evaluation of vascular access. Genereux et al. showed in a post hoc analysis of the 419 transfemoral patients from the Placement of AoRTic TraNscathetER Valves trial (PARTNER A and B) that vascular complications adversely impacted 30-day and one-year outcomes.1 In this analysis, major vascular complications (the most frequent being vascular dissection, vascular perforation and access site haematoma) occurred in as often as 15.4 % of cases with the use of the rst generation Edwards SAPIEN valves (Edwards Lifesciences Corporation, Irvine, California, US) and were associated with bleeding events, transfusions and increased mortality. Importantly, major vascular complications were associated with more than a fourfold increase in 30-day mortality.1 However, as shown by the Vancouver single-centre experience (137 patients), the incidence of major vascular complications can be dramatically reduced over time. Indeed, major vascular complications (22/24 were iliofemoral) in this centre fell from 8 % in 2009 to 1 % in 2010, thanks to increased operator experience, sheath size reduction (22 and 24 French size [Fr] for the rst Edwards SAPIEN generation as opposed to 19 and 18 Fr for the second generation) and improved screening using multislice computed tomography (MSCT).
access and management of its specic complications, but they should also perform comprehensive screening of patients and careful evaluation of vascular access. Genereux et al. showed in a post hoc analysis of the 419 transfemoral patients from the Placement of AoRTic TraNscathetER Valves trial (PARTNER A and B) that vascular complications adversely impacted 30-day and one-year outcomes.1 In this analysis, major vascular complications (the most frequent being vascular dissection, vascular perforation and access site haematoma) occurred in as often as 15.4 % of cases with the use of the rst generation Edwards SAPIEN valves (Edwards Lifesciences Corporation, Irvine, California, US) and were associated with bleeding events, transfusions and increased mortality. Importantly, major vascular complications were associated with more than a fourfold increase in 30-day mortality.1 However, as shown by the Vancouver single-centre experience (137 patients), the incidence of major vascular complications can be dramatically reduced over time. Indeed, major vascular complications (22/24 were iliofemoral) in this centre fell from 8 % in 2009 to 1 % in 2010, thanks to increased operator experience, sheath size reduction (22 and 24 French size [Fr] for the rst Edwards SAPIEN generation as opposed to 19 and 18 Fr for the second generation) and improved screening using multislice computed tomography (MSCT).
Furthermore, distinction between major and minor vascular complications is of importance since in the PARTNER trial, vascular subanalysis minor vascular complications, which occurred in 11.9 % of cases, were not associated with higher mortality, major bleeding, transfusions or need for dialysis at 30 days and one year.1
Vascular Screening
Using angiography and MSCT comprehensive vascular screening should determine the degree and localisation of calcications, the presence of relevant iliofemoral atherosclerotic disease, major tortuosity and the minimal lumen vessel diameter that must be at least >6 millimetres (mm) to accommodate an 18 Fr sheath. MSCT is very important in assessing the distribution of vascular calcication. Indeed, in the presence of circumferential calcication and/or tortuosity, the minimum iliofemoral arterial diameter should be larger (preferably >6.5 mm). In the setting of tortuous iliofemoral vessels the feasibility of transfemoral approach can be determined by the ability to straighten the tortuous vessel with a stiff wire (see Figure 1). Vavuranakis et al. developed an index to dene the signicance of vessel tortuosity - the Total arterial Tortuosity/Access vessel Diameter ratio (TT/AD). This ratio corresponds to the sum of angles from the puncture site divided by the minimum femoral artery diameter at the puncture site. In their analysis, a TT/AD >27.7 predicts major vascular complications with 50.8 % sensitivity and 70.6% specicity. This index, although not commonly used in clinical practice, supports the concept that larger arteries are less prone to vascular complications.2
Different 18 Fr Sheaths Used for the Medtronic CoreValve
Different 18 Fr sheaths are available when implanting a CoreValve (Medtronic Inc, Minneapolis, Minnesota, US). The Cook sheath (Cook Medical, Indiana, US) is 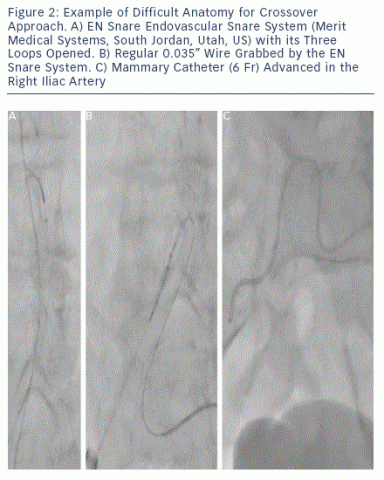 the most commonly used. It is robust enough to allow recapture of a partially deployed valve. The latter manoeuvre is more challenging when using the St Jude 18 Fr sheath (ST Jude Medical, Minnesota, US), which is softer and with a better prole, but has the tendency to invaginate during recapture of a partially deployed CoreValve.
the most commonly used. It is robust enough to allow recapture of a partially deployed valve. The latter manoeuvre is more challenging when using the St Jude 18 Fr sheath (ST Jude Medical, Minnesota, US), which is softer and with a better prole, but has the tendency to invaginate during recapture of a partially deployed CoreValve.
The recently available SoloPath™ Balloon Expandable sheath (Terumo Corporation, Japan) represents an interesting option in the presence of difcult vascular anatomy. The concept of this sheath is a reduced prole when folded (outer diameter of 13 Fr) allowing facilitated vessel entry, it is subsequently expanded by balloon ination up to an inner and outer diameter of 19 Fr and 22 Fr, respectively. It provides enhanced manoeuvrability, utilises the natural elasticity of vessels and thus enables delivery through difcult anatomy.3,4 Also, it is designed to collapse upon withdrawal. The SoloPath sheath is an interesting option for borderline iliofemoral access in terms of vascular diameter. However, caution should be paid in the presence of tortuous vessels because of a possibly limited kinking resistance observed in our preliminary experience.
Lubrification with Propofol
To facilitate large bore sheath insertion in calcied vascular access, lubrication of the sheath with sterile propofol may be of help. This tip and trick was also successfully described in the case of stent delivery failure in coronary arteries.5 Indeed, propofol is a short-acting intravenous hypnotic/amnestic agent with lubricating properties, as it is an emulsion of 1.0 % propofol, 10.0 % soybean oil, 1.2 % puried egg phospholipids, 2.25 % glycerol and sodium hydroxide.
Pre-closure Technique Using the Prostar 10XL Device
Surgical femoral cut-down may at rst glance seem safer than a fully percutaneous approach. However, surgery may be associated with adverse events such as haematoma, seroma, lymphoceles and infection, and may lengthen the intervention, the timing to ambulation and hospital stay.6 On the other hand, a fully percutaneous approach has been used for many years in the eld of endovascular aortic aneurysm repair and has the advantage of being performed under local anaesthesia with mild sedation. At present, with the reduction of sheath size, many centres favour this latter approach.
At the beginning of the procedure, the sutures of the Prostar device are deployed at the arteriotomy site without tying the knots. At the end of the procedure, the sutures of the pre-closing system are knotted while retrieving the large sheath using either the crossover balloon technique (see below) or with a crossover access to the external iliac artery ready in case of incomplete haemostasis. Failure of the Prostar XL device seems to be associated with obesity, small-diameter vessels with signicant calcication or a high puncture site.8-10 The failure rate of the Prostar device has been reported to be between 7.4 and 15.0 % in TAVI and endovascular aortic aneurysm repair series.6,10-12 In a series of 142 patients from Paris, the rate of failure clearly decreased from early experience (14.3 %) to later experience (4.3 %) whereas the total failure rate was 9.4%.10 Interestingly, in this series, all Prostar failures could be managed without surgical intervention, namely with prolonged balloon ination (3.6 %) or covered stent implantation (3.6 %) and no Prostar failure led to a major vascular complication according to the Valve Academic Research Consortium (VARC) criteria.10
Crossover Balloon Occlusion Technique
Some operators routinely advance a peripheral balloon in the external or common iliac artery from the contralateral access and inate it when retrieving the sheath 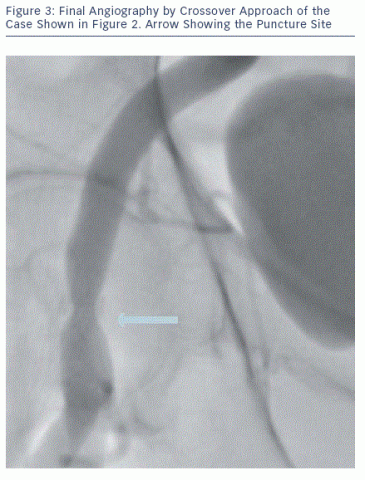 and knotting the sutures - the so-called crossover balloon occlusion technique. This approach permits bleeding control and offers a bloodless eld for percutaneous or surgical repair if needed.9,13 In our experience, the need to inate a balloon to achieve haemostasis is rarely needed and we therefore do not use it prophylactically. However, we strongly advise having a diagnostic catheter in place in the external iliac artery using a contralateral approach. This can be easily done by advancing a 6 Fr internal mammary artery catheter over a 0.035" wire (usually a stiff Terumo wire, Terumo Inc, Japan). If the aortic bifurcation is narrow-angled and it is not possible to easily advance a wire into the contralateral limb, we advise snaring it (e.g. with EN Snare® Endovascular Snare System [Merit Medical Systems, South Jordan, Utah, US]) from the large bore introducer site. This technique may be the only way to 'secure' the contralateral limb in challenging cases (see Figure 2). From the 6 Fr mammary, an angiogram is performed to document complete haemostasis at the Prostar site (see Figure 3).
and knotting the sutures - the so-called crossover balloon occlusion technique. This approach permits bleeding control and offers a bloodless eld for percutaneous or surgical repair if needed.9,13 In our experience, the need to inate a balloon to achieve haemostasis is rarely needed and we therefore do not use it prophylactically. However, we strongly advise having a diagnostic catheter in place in the external iliac artery using a contralateral approach. This can be easily done by advancing a 6 Fr internal mammary artery catheter over a 0.035" wire (usually a stiff Terumo wire, Terumo Inc, Japan). If the aortic bifurcation is narrow-angled and it is not possible to easily advance a wire into the contralateral limb, we advise snaring it (e.g. with EN Snare® Endovascular Snare System [Merit Medical Systems, South Jordan, Utah, US]) from the large bore introducer site. This technique may be the only way to 'secure' the contralateral limb in challenging cases (see Figure 2). From the 6 Fr mammary, an angiogram is performed to document complete haemostasis at the Prostar site (see Figure 3).
Crossover Final Angiography
It is essential to perform a nal angiography of the vascular access by a crossover approach to verify the haemostasis and to exclude local complications such as dissection or vessel occlusion. Small leaks are not seen from the skin and they may contribute to the formation of a false aneurysm or become the source of delayed major bleeding. If small vascular leakages are seen, prolonged manual compression is usually effective in sealing the leak and a nal angiographic check is required to conrm the sealing. Large leaks or tears often require covered stenting or surgical intervention. In this setting, proximal balloon occlusion is a valuable bridge to endovascular or surgical repair.
In summary, careful patient screening associated with device size reduction and expertise in advanced percutaneous techniques should result in very low complication rates when using the transfemoral approach, even for fully percutaneous procedures. Most local complications can be treated by endovascular methods, surgery is rarely needed.