High-risk Subgroups for Bleeding and Vascular Complications
Patients undergoing PCI in the context of ACS are expected to receive a combination of potent multiple antithrombotic drugs that may lead to an increased risk 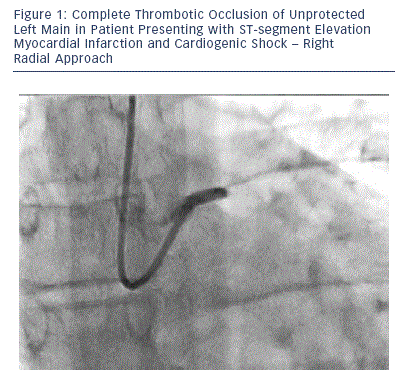 of bleeding and subsequent morbidity and mortality.
of bleeding and subsequent morbidity and mortality.
Women are at higher risk of bleeding and other adverse outcomes after PCI than men.34,35 In a recent observational study, routine TRA was associated with reduced bleeding risk in women.36 Unfortunately, muscular arterial hyper-reactivity, procedural discomfort and small artery diameter increases the risk of rst radial access failure (9.6% in women versus 1.6 % in men). However, successful radial access does not allow the operator to use more aggressive combinations of anticoagulants and antiplatelet agents in this group, given that women remain at higher non-access site bleeding risk.37,38
Elderly patients are also at high risk for bleeding and vascular complications post-PCI. Lower limb peripheral artery disease (PAD), tortuosity of the iliac arteries and aneurysms of the abdominal aorta may represent relative or absolute contraindications to TFA. As a result of PAD in the elderly, radial access appears to be as feasible as femoral access. In two randomised trials, the TRA was associated with fewer vascular complications in elderly patients.39,40
Cardiogenic Shock and Left Main Culprit in Acute Coronary Syndrome
Cardiogenic shock has a poor outcome compared with less severe presentations of ACS. The Should We Emergently Revascularize Occluded Coronaries for Cardiogenic Shock (SHOCK) trial40 showed the importance of revascularisation to improve outcomes, but the recent Intraaortic Balloon Pump in Cardiogenic Shock II (IABP-SHOCK II) trial41 failed to 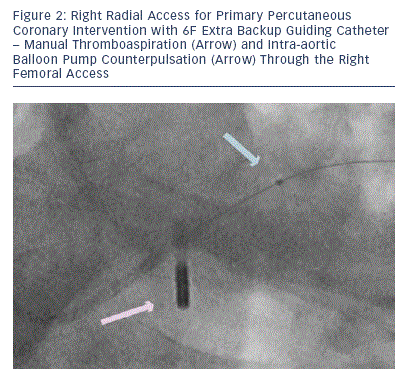 show any marginal benet of adding haemodynamic support with intra-aortic balloon counterpulsation in the setting of shock.
show any marginal benet of adding haemodynamic support with intra-aortic balloon counterpulsation in the setting of shock.
Cardiogenic shock is associated with a doubling of the risk of bleeding compared with the absence of shock.42 There may be a safety advantage of using the radial artery for the coronary intervention and reserving the femoral artery for larger devices in patients with cardiogenic shock (see Figures 1-4).
Rodriguez-Leor analysed their single-centre registry experience with radial access in cardiogenic shock patients. From a 1,400-patient experience, 122 (8.7 %) developed cardiogenic shock with 80 undergoing transfemoral and the remaining 42 undergoing transradial catheterisation. Mortality (64.3 versus 32.5 %, p<0.001), serious access site complications (11.9 versus 2.5 %, p<0.03), access site complications requiring blood transfusion (7.1 versus 0.0 %, p<0.04) and MACCE (death, infarction, stroke, serious bleeding and postanoxic encephalopathy) (73.8 versus 43.8 %, p<0.001) were greater in patients treated by the femoral route. After multivariate analysis, initial TRA was associated with lower mortality (OR 0.39; 95% CI 0.15-0.97) compared with an initial TFA.43
Bernat et al. evaluated outcomes of 197 STEMI patients with signs of cardiogenic shock who were treated with primary PCI at two highvolume centres. The TRA was used successfully in 55 % of cases where at least one radial artery was weakly palpable. TRA emerged as an independent predictor of survival with more than half of the patients treated successfully. Mortality at one-year was 44 % in the radial group and 64 % in the femoral group (p=0.0044).44
Romagnoli et al. analysed 241 consecutive patients (91 % with ACS and left main culprit in 26 % of cases) receiving IABP support during PCI in four high-volume centres. Patients were further divided in two groups - 116 patients receiving double femoral access (FF) and 125 receiving both radial and femoral (RF) approaches. NACEs were more frequent in the FF group when compared with the RF group (67 versus 41%, p<0.01). In particular, this difference originated from an increase of access site-related bleeding (21 versus 7 %, p<0.01) and cardiac death (41 versus 25%, p<0.01).45 These data show that a radial-femoral access strategy is safer than a femoral-femoral access strategy, and this safety advantage is associated with reduced mortality.45
Left Main Culprit
A signicant involvement of the left main coronary artery occurs in 4-7 % of patients presenting with an acute myocardial infarction (AMI).46,47 These critically ill 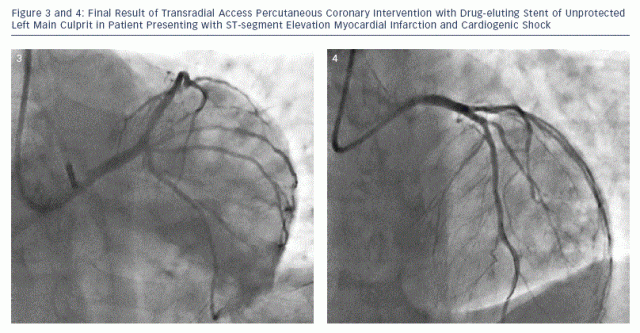 patients frequently present with cardiogenic shock or cardiac arrest and are at high risk for in-hospital major cardiac adverse events.48,49
patients frequently present with cardiogenic shock or cardiac arrest and are at high risk for in-hospital major cardiac adverse events.48,49
Primary PCI for an AMI due to an unprotected left main coronary artery (ULMCA) culprit lesion is a rare procedure, frequently associated with adverse clinical outcomes. The incidence of AMI due to an ULMCA culprit lesion is reported to be 0.8-5.4 %.50
Patients undergoing primary PCI for an AMI due to an ULMCA culprit lesion and presenting with cardiogenic shock have a high 30-day mortality compared with patients without cardiogenic shock, with the estimated 30-day all-cause mortality of 55 % for patients with cardiogenic shock and 15 % for patients without cardiogenic shock. A hybrid approach of initial revascularisation by primary PCI and elective surgery afterwards remains an alternative treatment option.
Treating patients with cardiogenic shock or after cardiac arrest is one of the most challenging PCI procedures due to the nature of the clinical presentation while targeting a coronary lesion associated with a very large area of the myocardium at risk. These haemodynamically unstable patients have an extensive amount of ischaemic myocardium. Immediate mechanical haemodynamic support may prevent from further multi-organ failure.
Whether newer and more powerful circulatory assist devices (Impella®, TandemHeart®, Extracorporeal Membrane Oxygenation [ECMO]) will result in better outcomes is the subject of ongoing clinical evaluation before widespread adoption.51
Most PCIs in high-risk ACS patients can be performed by TRA through conventional 6 French (Fr) guiding catheters, including complex cases, left main bifurcations and cardiogenic shock. However, a stepwise approach to learning is proposed and high-risk ACS-PCI is recommended as the last step.
Ultimately, the treatment of patients in shock requires an individualised approach. Although the radial pulse may return with vasopressor administration, there may be clinical situations in which radial access is not possible and femoral access must be used. From the available evidence supporting the safety of the TRA over the TFA, a 'radial rstÔÇÖ strategy likely still applies in most patients, even those with large STEMI and shock if performed by a skilled and experienced radial operator. Haemodynamic support devices can be placed via the femoral route and temporary pacemakers can be placed through the forearm or femoral veins (see Figures 1-4).52