 Patient Selection
Patient Selection
LVAD therapy should be considered in every patient with end-stage systolic (low LV ejection fraction) HF who has no other life-limiting diseases. Tables 1 and 2 summarise the current MCS recommendation from the AHA and the ESC. Table 3 details the indications and contraindication for MCS.
A MCS evaluation is essential to identify those patients who could benefit from device implantation, and to exclude those considered futile for device therapy. The first step in patient selection is to accurately estimate the clinical severity of the HF syndrome. Many US clinicians22 recommend the use of two prognostic scores, the Heart Failure Survival Score23 and the Seattle Heart Failure Model,24 to estimate the expected two-year survival on medical therapy in candidates who might benefit from LVAD support.22 The ESC recommend assessing the patient’s prognosis using variables that have been shown to predict outcome, such as findings in history and physical examination (NYHA class, blood pressure, signs of congestions, etc.), laboratory tests (serum sodium, liver enzymes, troponins, etc.), neuro-hormonal activity (Plasma renin activity, Angiotensin II, etc.), and functional (peak VO2) and haemodynamic variables.10,21 Likewise, it is now apparent that there are many phenotypes of advanced HF, which have been described with the INTERMACS profiles, a classification of 7 clinical profiles (see Table 4).25 Patients with INTERMACS profile 1 to 3 are being managed with temporary mecha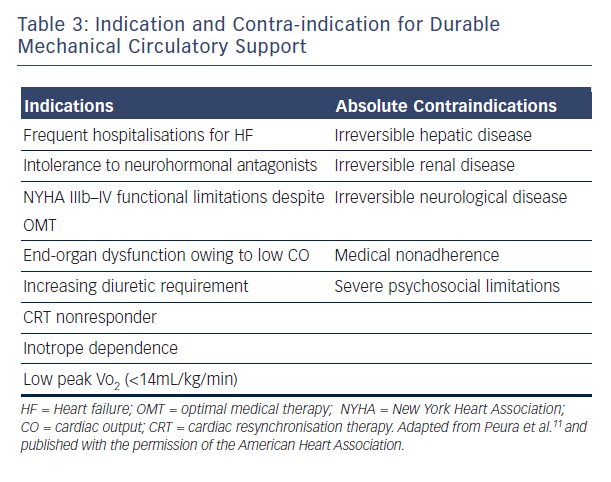
For example, INTERMACS profile 1 or 2 patients who 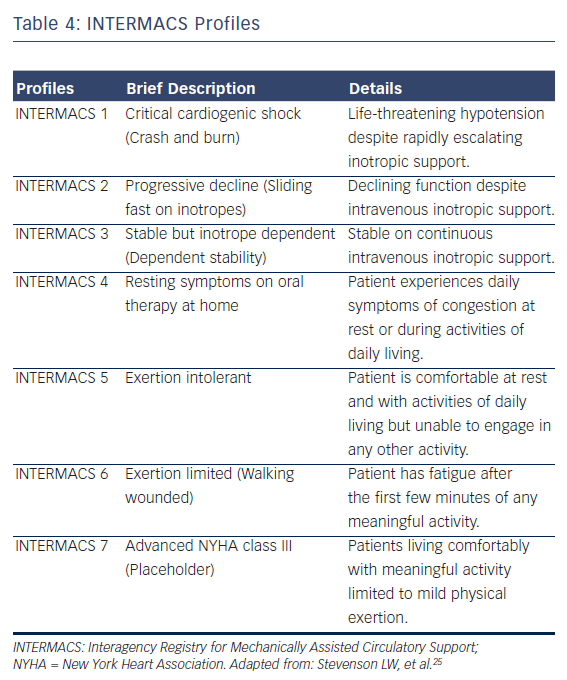
The ‘Lietz-Miller score’ was the most frequently used risk score for DT patients (see Table 5)28, but is now limited in use as it was developed on the first generation HeartMate XVE device.28
The second step in the evaluation is to search for significant co-morbidities and other factors that might limit the patient’s suitability.11 This search should include the possibility of reversible causes of heart failure (for example: obstructive sleep apnoea), metabolic stress testing when feasible (stress tests are contra-indicated in patients on inotropes), invasive haemodynamic evaluation, laboratory 
All patients should undergo a psychosocial evaluation to estimate patient psychological status, risk for substance abuse, compliance to treatment and
supporting environment.22,29
Right ventricular (RV) failure is a leading cause of mortality after LVAD implantation,22 since LVAD optimal function relies on adequate filling of the left ventricle (LVAD preload), which in turn is dependent on RV function. Many studies have tried to predict which patients are at risk for RV failure after LVAD implantation.30–36 Table 6 summarises the major published predictors of post implant RV failure.
The final step in evaluating LVAD candidates is an estimation of a patient’s overall frailty. Frailty was originally a geriatric term defined as a state of vulnerability to adverse outcomes and decreased physiologic reserve, reflecting the biologic rather than chronologic age.37,38 Frailty is very common among HF patients and adversely affects prognosis39,40. In LVAD patients, frailty is associated with higher post-implant complication rates and mortality.38,41
LVAD Complications
Patients treated with long-term MCS may develop characteristic complications associated with the implantation of the VAD.