Prognostic Value of hsTn
With the development of hsTn assays and the detection of cTn at extremely low levels, a detectable troponin level has continued to show prognostic value in patients with AHF. Yue et al were the first to study serial hsTn I (hsTnI) measurements in patients admitted with AHF, using the highly sensitive VerisensTM RUO Human cTnI assay (Nanosphere). In this study of 144 serial patients presenting with AHF, hsTnI was assessed from admission to discharge with follow-up at 90 days for heart failure-related readmission and mortality.35 Nearly every patient had a troponin level detected above the limit of detection of the assay. Patients with increasing hsTnI levels during 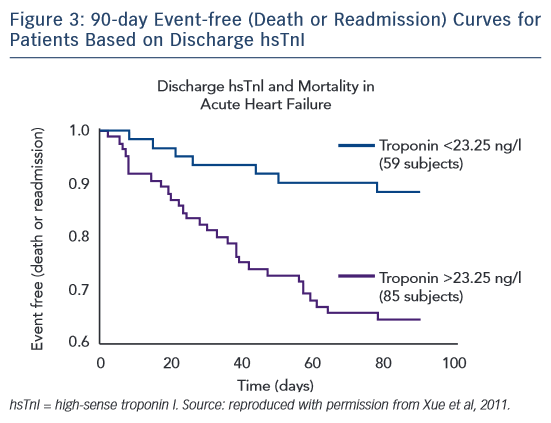 treatment had a higher mortality rate than those with a stable or decreasing hsTnI level. Patients with a discharge hsTnI level >23.25 ng/l had an increased risk of readmission and mortality (Figure 3). In an analysis of the ASCENDHF trial, an hsTnI level >0.034 ng/ml on admission was associated with an increased risk of in-hospital mortality, worsening heart failure during admission, and increased length of hospital stay in the first 7 days, but not long-term outcomes at 30 or 180 days.36 A subset of patients had hsTnI measurements taken on admission and 48–72 hours later. Patients with a 20 % increase in hsTnI level had increased risk of 30-day mortality and in a logistic regression model the hsTnI value at 48–72 hours was associated with 30-day mortality, but not the value at admission.
treatment had a higher mortality rate than those with a stable or decreasing hsTnI level. Patients with a discharge hsTnI level >23.25 ng/l had an increased risk of readmission and mortality (Figure 3). In an analysis of the ASCENDHF trial, an hsTnI level >0.034 ng/ml on admission was associated with an increased risk of in-hospital mortality, worsening heart failure during admission, and increased length of hospital stay in the first 7 days, but not long-term outcomes at 30 or 180 days.36 A subset of patients had hsTnI measurements taken on admission and 48–72 hours later. Patients with a 20 % increase in hsTnI level had increased risk of 30-day mortality and in a logistic regression model the hsTnI value at 48–72 hours was associated with 30-day mortality, but not the value at admission.
Assays using hsTn T (hsTnT) also have prognostic value similar to that of hsTnI. In a study of 202 patients with AHF, conventional cTnT and hsTnT assays were performed and patients were followed-up for >1 year for mortality.37 Both cTnT and hsTnT had predictive value for death. In patients with a cTnT level <0.03 ng/ml, the addition of a positive hsTnT value, especially if greater than 20 pg/ml, improved risk prediction of death over clinical factors alone. In another study, 113 patients with AHF and a conventional cTnT test result below the cutoff of 0.03 ng/ml on admission were enrolled.38 An elevated admission hsTnT level, especially if >77 pg/ml, was found to be a significant predictor of death, and retained this significance in multivariate analysis with HR of 1.003. In a retrospective analysis of 100 patients admitted with AHF and hsTnT values measured on days 1 and 3, patients in whom the hsTnT levels decreased were found to respond to therapy and return to a compensated state, while those whose hsTnT levels did not change remained decompensated.39 In addition, patients in whom hsTnT levels increased during this time had longer durations of hospitalisation. As hsTn assays become more widely used, these studies demonstrate that in patients with AHF hsTn retains prognostic use similar to conventional cTn assays.